Hello friends!
I hope you had a wonderful long weekend with your loved ones!
As we do each week, we will review the bad news, the good news, the most commonly asked questions of the week and end on my silver lining.
What is the bad news?
There have been over 500 MILLION cases of COVID reported worldwide, with at least 6.2 million deaths.
Over 3.6 million cases have been reported in Canada, with over 38,200 deaths. There are at least 205,000 active cases of COVID in Canada right now. This is a significant underestimate as only PCR tests are included in this count.
Over 5,500 people are hospitalized in Canada now due to COVID. This has increased by over 1,000 since last week.
We are well into wave six now, driven by the more transmissible BA.2 variant. Waning immunity and lifting public health measures such as masking lead to rapid spread.
According to modelling from the Ontario Science Table, hospital admissions will likely continue to rise. It is unclear when and how high it will peak.
COVID infections in healthcare workers are as high as in the last Omicron wave. The graph here only includes health care workers with positive PCR tests. Rapid tests were excluded. Therefore, the actual number of infected healthcare workers is considerably higher. High infection rates in health care workers are stressing hospital operations and may decrease the ability to provide health care services. The burnout many providers have felt over the last two years stresses a vulnerable system.
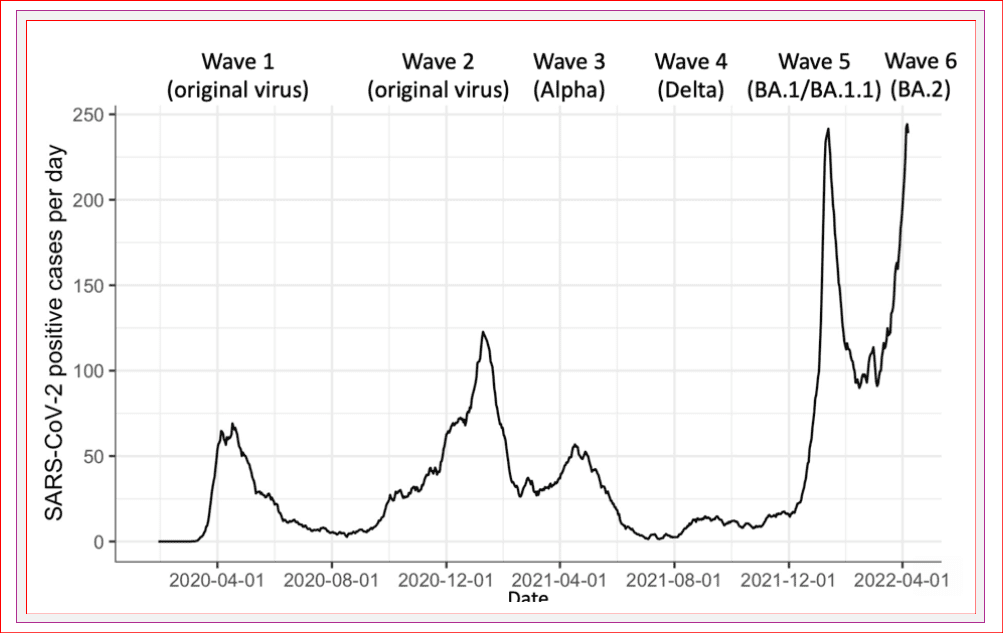
Resource – Ontario Science Table
What do we know about Long-COVID?
Long-COVID or ‘post-COVID-19 condition’ occurs in individuals with a history of COVID-19 infection, typically within the last three months, with symptoms lasting over two months with no alternative diagnosis. Any person who has had COVID is at risk of developing long COVID.
The most common symptoms we see are fatigue, shortness of breath and cognitive dysfunction. Many people have disruptions in work, school or family life. This adds a burden on the stressed health care system.
Conservative estimates suggest that at least 10% of all unvaccinated people infected with COVID-10 will develop Long-COVID. There are no medications or treatments available to prevent long-COVID or treat it. Preventing infection with public health measures and vaccination is the only current strategy.
We do not yet know the impact of long-COVID on kids.
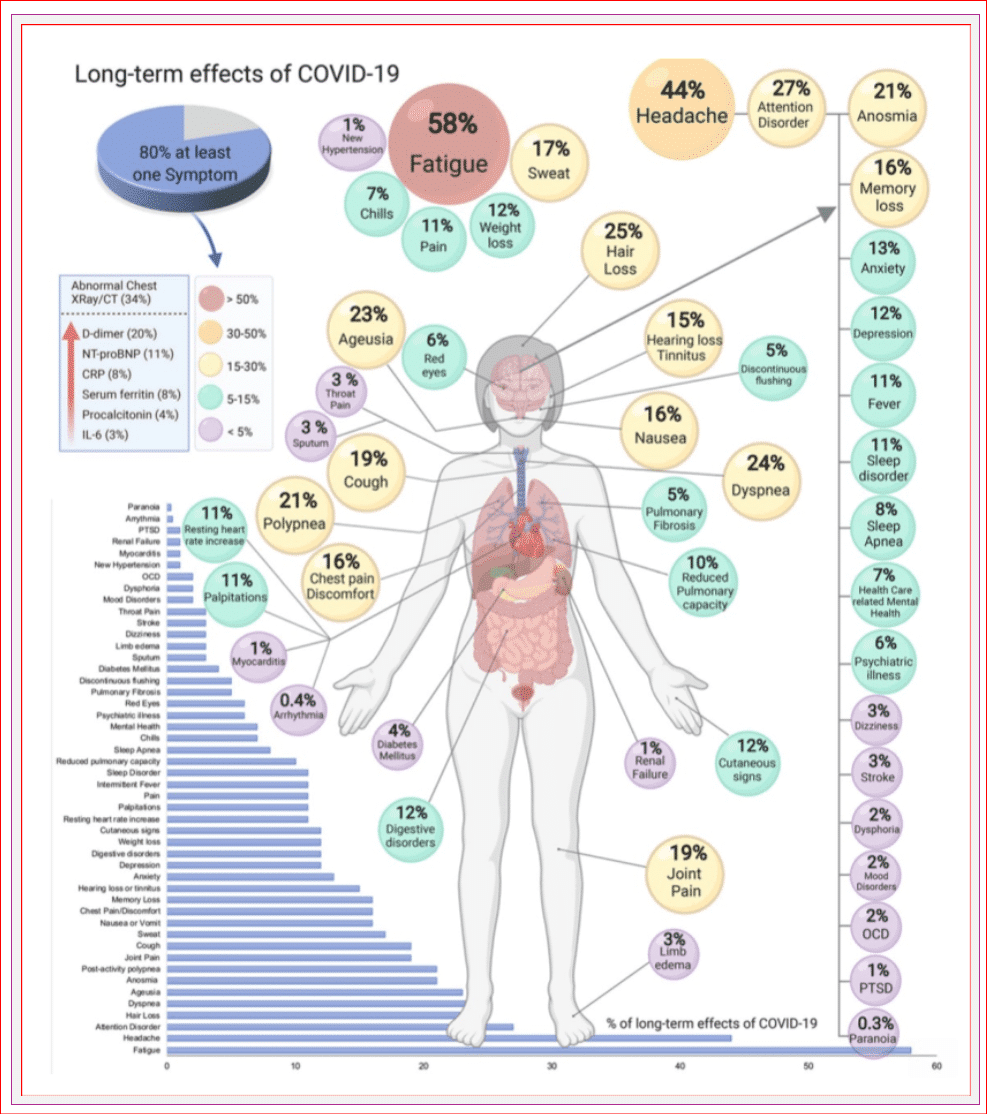
Multiple research papers demonstrate a link between COVID infection and other illnesses such as psychiatric conditions, neurological disease, diabetes, and heart disease. The risk of heart attacks and strokes has increased substantially, particularly for those who experience severe COVID illness.
The most common questions of the week
What does infection from Omicron look like?
The most common symptoms of Omicron infection are:
- Runny nose or sneezing
- Sore throat
- Cough
- Headache
- Fever
- Vomiting or diarrhea
- Loss of smell
Do rapid antigen tests work for Omicron?
Rapid antigen tests (RAT) are not as sensitive to Omicron as previous strains.
According to the Ontario Science Table:
- During the first three days after symptoms start, rapid antigen tests SHOULD NOT be used to rule out an infection.
- If you have symptoms, stay home and isolate yourself.
- At least two negative RATs should be done, at least 24 hours apart, to be confident you don’t have COVID.
- Swab multiple areas for a more reliable test.
- Swab the throat on each side, the inside of the cheeks on each side, the back of the tongue, AND each nostril, to get the best sample.
COVID is everywhere – how can I prevent infection?
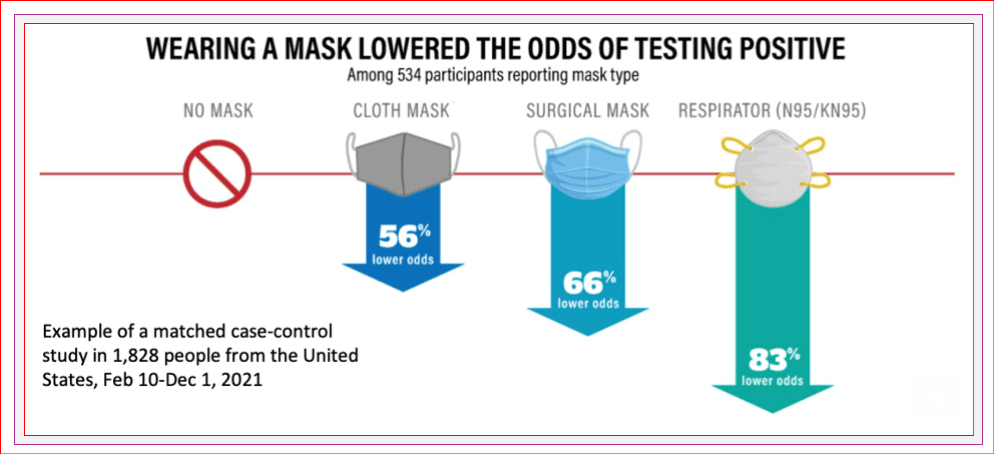
While no longer required in most settings, I still strongly recommend wearing a well-fit mask in public. This is based on strong evidence that wearing a properly fitted quality mask prevents COVID transmission. Masking protects the person wearing the mask and the people around them.
Masking in indoor areas substantially reduces the risk of getting and spreading COVID. Improvements to ventilation help as well. The more people who wear masks in public, the more our community benefits from less circulating COVID.
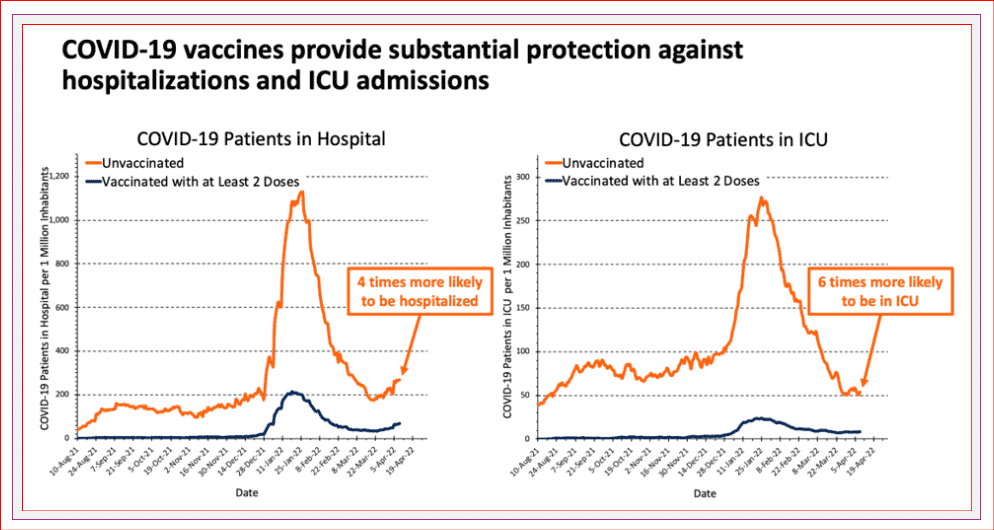
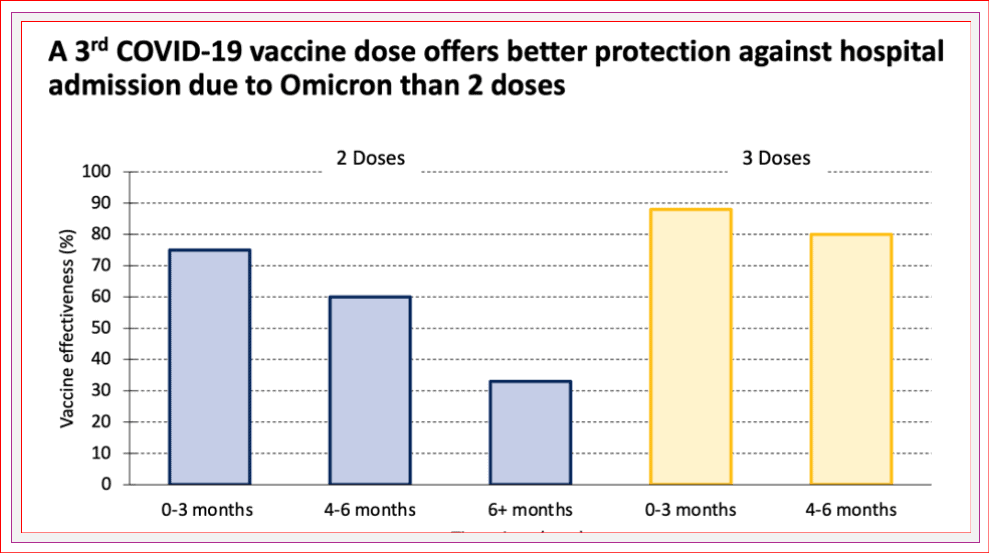
Do vaccines still help?
Having a complete vaccine series (2 doses in kids, 3 in adolescents and adults and 4 in older adults and high-risk individuals) is very helpful in preventing severe illness requiring hospital or ICU admission and death, and reduces the likelihood of developing COVID, if you do get infected. In adults, boosters help more than having only two doses.
Who can get COVID antivirals now?
You may have heard that some pharmacies have the antiviral medication Paxlovid. Individuals at high risk of severe outcomes from COVID are advised to seek testing and an assessment.
Those at high risk include:
- Aged 18+ and immunocompromised
- Aged 70+
- 60+ with fewer than three vaccine doses
- Pregnant and unvaccinated
- 18+ with fewer than three vaccine doses and at least one risk condition (obesity, diabetes, or heart disease).
These individuals also qualify for PCR testing. Physicians can prescribe Paxlovid directly to higher-risk patients with symptoms and a positive COVID-19 test (PCR or RAT).
Paxlovid must be started within five days of symptoms.
Paxlovid is available through both COVID clinical assessment centres and some community pharmacies.
Will boosters of Pfizer be available for 5-11-year-olds soon?
Pfizer is currently looking for approval for its booster shot for kids aged 5-11.
A small study in the United States involving 140 children showed that a Pfizer booster given six months after receiving a second dose of the Pfizer vaccine increased the children’s immune responses. The Pfizer vaccine is approved in children aged five to 11 as part of their primary series, not as a booster shot in Canada. I will update you if/when the booster shot is approved for this age group.
My silver lining of the week
The weather is warming, and the birds are chirping. As our four-year-old says, ‘you can tell Spring is almost here when the flowers come out.’
Have a great, healthy, week.

![[Dr. Dina News] IMPORTANT UPDATE re. VIRTUAL CARE](https://drdina.ca/wp-content/uploads/2021/01/dr-dina-kulik-kids-and-virtual-care-1a-400x250.jpg)
![[Dr. Dina News] COVID-19 Vaccine for Infants and Young Children.](https://drdina.ca/wp-content/uploads/2021/04/dr-dina-kulik-kids-and-vaccines-400x250.jpg)
![[Dr. Dina News] COVID-19 Vaccine for Infants and Young Children.](https://drdina.ca/wp-content/uploads/2022/04/DRD-1-400x250.jpg)






